Resonancia magnética de los senos
encontrar mi
¿Qué es una resonancia magnética de mama?
La resonancia magnética, también llamada resonancia magnética, es una prueba de radiología que utiliza potentes imanes y ondas de radiofrecuencia para generar una imagen detallada de los huesos, tejidos blandos (músculos, tendones, etc.), órganos y otras partes del cuerpo. La prueba no utiliza ninguna radiación. Una resonancia magnética de mama es una resonancia magnética que se realiza con una máquina especial que tiene herramientas para tomar imágenes detalladas de las mamas.
¿Para qué se utiliza la resonancia magnética de mama?
La resonancia magnética de las mamas puede ayudar a los proveedores a aprender más sobre la salud de sus senos y puede ayudar a encontrar problemas que no se pueden ver en una mamografía o una ecografía. La resonancia magnética no debe reemplazar una mamografía y las pruebas a menudo se usan juntas. Cada prueba puede encontrar diferentes problemas en el tejido mamario. Algunos proveedores sugieren alternar las pruebas cada seis meses, mientras que otros ven un beneficio en leerlas juntas. Su proveedor podrá decirle cuándo debe realizarse cada prueba.
La resonancia magnética de mama tiene muchos usos, como:
- Detección de cáncer de mama para mujeres con alto riesgo de padecer cáncer de mama debido a antecedentes familiares o a su propia historia de salud.
- Para comprobar los resultados de una mamografía que necesitan más pruebas.
- Evaluar un nuevo diagnóstico de cáncer.
- Como seguimiento después del tratamiento del cáncer de mama.
- Para revisar implantes mamarios que puedan haberse roto.
¿Cómo me preparo para el examen?
Por lo general, no existe una preparación especial para una resonancia magnética de mama. A menos que le indiquen lo contrario, puede comer y beber como lo haría normalmente. Es mejor dejar joyas, perforaciones corporales, pinzas para el cabello y otros metales en casa, ya que no están permitidos en la sala de resonancia magnética. Informe al técnico si tiene algún metal en el cuerpo, como un desfibrilador/marcapasos, un cateterismo portátil u otros implantes metálicos.
Si tiene claustrofobia (no le gustan los espacios reducidos), es posible que necesite tomar medicamentos para relajarse antes de la prueba. Hable con su proveedor de atención médica si tiene alguna inquietud.
¿Cómo se realiza el examen?
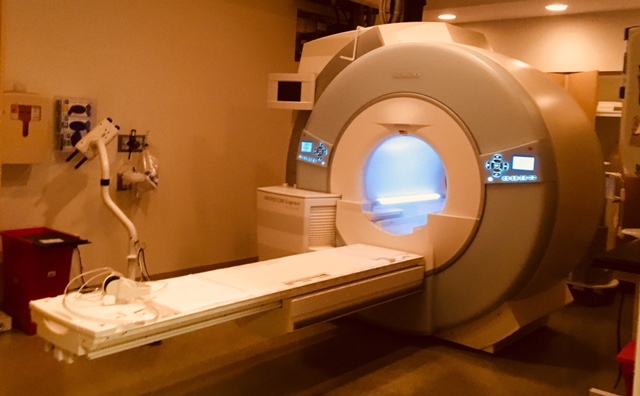
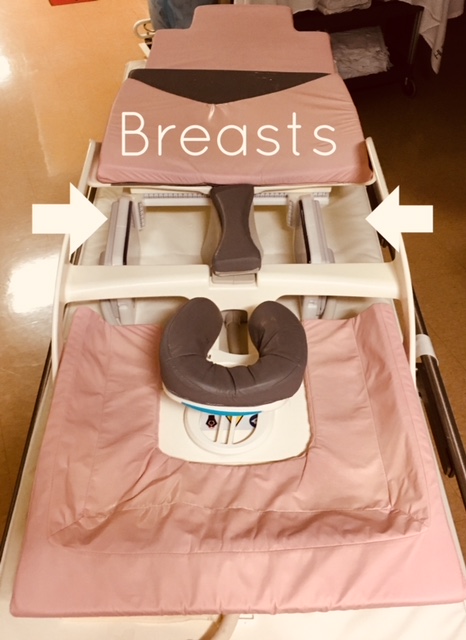
Una resonancia magnética de los senos utiliza una mesa con orificios para los senos. Te acostarás boca abajo sobre la mesa, con los senos colgando por los agujeros. Esto permite observar el tejido mamario sin apretarlo como en una mamografía. La máquina puede presionar sus senos para evitar que se muevan. Deberá permanecer acostado e inmóvil durante la prueba, por lo que es importante que se sienta cómodo. La mesa se desliza dentro de un tubo y los imanes giran a tu alrededor. La resonancia magnética es ruidosa, por lo que es posible que le den auriculares o tapones para los oídos para ayudar a bloquear el ruido.
La resonancia magnética de mama casi siempre utiliza un contraste (tinte) administrado por vía intravenosa (IV) llamado gadolinio. No tendrá contraste si la resonancia magnética busca implantes rotos. El contraste se aplicará antes de la prueba. La prueba completa puede durar entre 45 y 60 minutos.
¿Qué es una resonancia magnética mamaria rápida?
La resonancia magnética mamaria rápida, también llamada resonancia magnética mamaria abreviada, a veces se usa junto con una mamografía para mujeres con tejido mamario denso que no cumplen con los requisitos para una resonancia magnética mamaria completa. No puede encontrar tanto como una resonancia magnética de mama completa, pero es buena para detectar cáncer de mama invasivo. La prueba se puede realizar en tan solo 10 a 15 minutos. Muchos planes de salud no pagan por esta prueba. Es posible que tengas que pagar de su bolsillo la prueba, que normalmente cuesta entre 300 y 400 dólares.
¿Quién debería hacerse una resonancia magnética de mama?
Las mujeres con alto riesgo de cáncer de mama deben realizarse una resonancia magnética de mama. Las pautas de detección del cáncer de mama de la Sociedad Estadounidense del Cáncer (ACS) sugieren una prueba de resonancia magnética anual, junto con una mamografía, para las siguientes mujeres:
- Aquellos con una mutación (genética) BRCA 1 o 2 conocida.
- Mujeres que no se han realizado pruebas genéticas, pero tienen un familiar de primer grado con una mutación BRCA (hermana, madre, hija).
- Mujeres con un riesgo previsto de por vida del 20 % al 25 % o más de sufrir cáncer de mama (determinado mediante el uso de herramientas de evaluación de riesgos; más información a continuación).
- Mujeres que recibieron radiación en el pecho entre las edades de 10 a 30 años.
- Mujeres con ciertos síndromes genéticos o un familiar de primer grado con el síndrome (Cowden, Li-Fraumeni, Bannayan).
Algunas mujeres se consideran de alto riesgo de sufrir cáncer de mama, pero no forman parte de los grupos anteriores. Estos incluyen mujeres con:
- Riesgo previsto de por vida de menos del 20%, pero más del 15%.
- Aquellos con antecedentes de carcinoma lobulillar in situ (CLIS), hiperplasia lobular atípica o ductal.
- Alta densidad mamaria (tejido mamario denso) en una mamografía.
Pregúntele a su proveedor si debe hacerse una resonancia magnética de mama y cuándo. También puede obtener más información sobre su riesgo de cáncer de mama aquí:
- Riesgo y prevención del cáncer de mama
- Cómo el historial de salud de una mujer afecta el riesgo de cáncer de mama
¿Qué pasa con el costo?
Una resonancia magnética es más costosa que una mamografía. La cobertura de las compañías de seguros será diferente y probablemente dependerá del riesgo de la mujer. Asegúrese de verificar su cobertura con su compañía de seguros antes de realizarse una resonancia magnética de mama.
No todas las clínicas cuentan con máquinas de resonancia magnética mamaria ni proveedores que puedan leer los resultados. Es importante hablar con su proveedor sobre si esta es una prueba que debe realizarse y cuál es el mejor lugar para realizarla.